The healthcare credentialing process has hundreds of moving parts and details that must all align for a provider to be enrolled with payers and gain necessary privileges. Enhanced credentialing reporting helps to keep the process moving, identify areas of improvement, and provide visibility to leadership.
MedTrainer Credentialing Software offers customizable dashboards and credentialing reports that give healthcare teams the insight needed to protect revenue and patients.
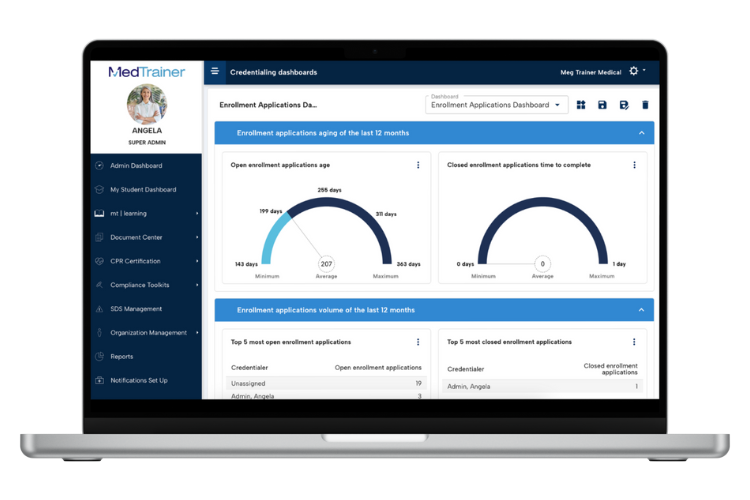
Customizable Credentialing Dashboards
MedTrainer credentialing dashboards offer an in-depth look at your organization’s payer enrollment process. Choose the data you want to see and how you’d like it visualized — graph, chart, pie, or gauge.
Your team can use this data to more accurately project timelines, identify process improvements, and more. Many teams use credentialing dashboards to identify applications that are not being handled by a credentialer, know if a payer or provider is likely to delay progress, and even to identify top credentialers so others can learn from their success.
Here are some of the most popular dashboards:
| Data Set | What It Tells You |
| Application Assignments |
|
| Application Aging |
|
| Application Status |
|
| Application Process by Payer |
|
| Application Process by Provider |
|
| Application Volume |
|
| Follow-Up Status |
|
Learn more in 5 Key Provider Enrollment Metrics You Can Use To Accelerate Revenue.
Quickly Identify Missed Enrollments
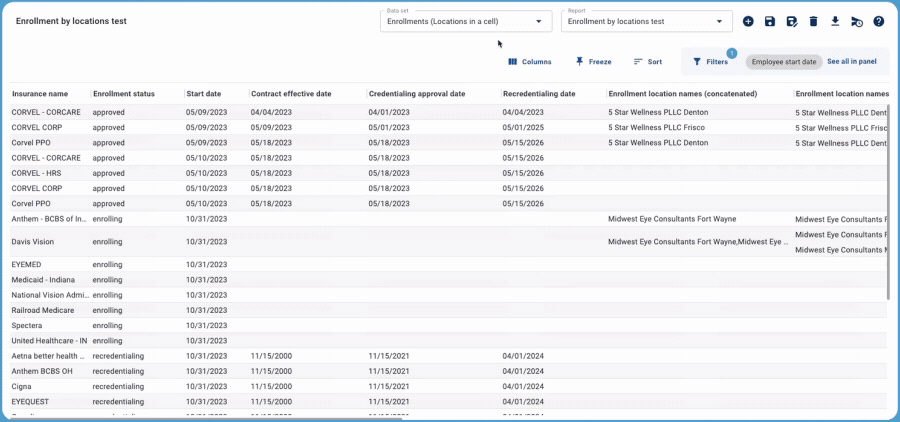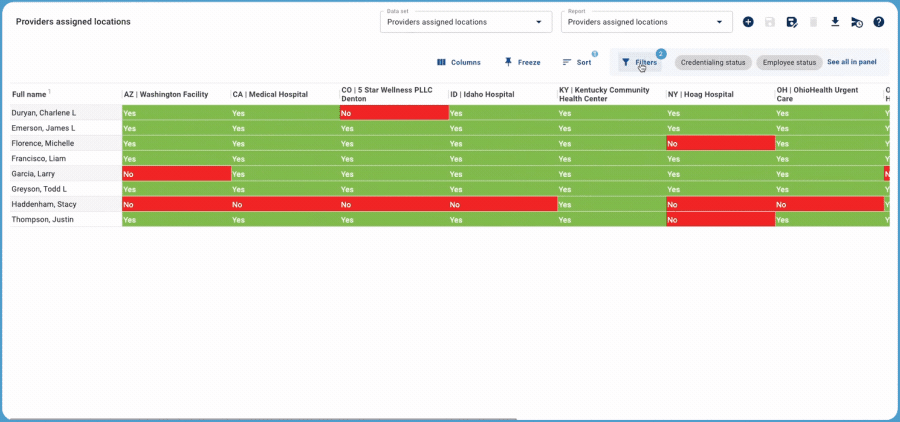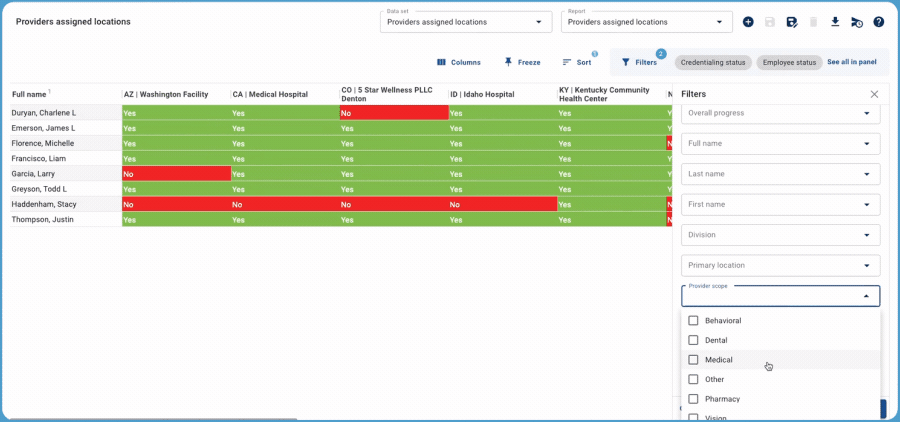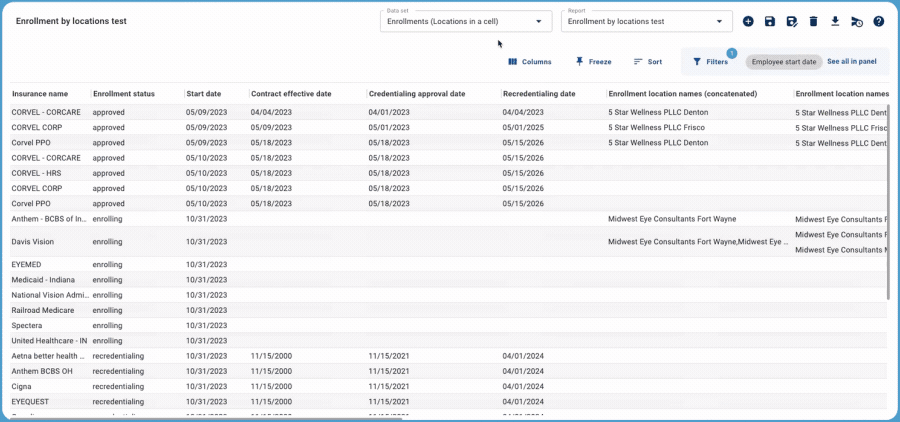
When every provider in your organization is enrolling with 10-25 different payers, one application can easily slip through the cracks — with costly impacts. MedTrainer’s pivot data sets make it easy to identify missed enrollments. The key is that the pivot table shows a “pattern” that can quickly be understood.
For example, when the data shows that every medical provider is enrolled with a specific payer (green cells), the one outlier is literally a red flag. In seconds, you have identified the needle in the haystack and can quickly work to correct the issue. When all your cells are green, you know at a quick glance that all enrollments are complete. If your organization has multiple locations, you can also use the pivot tables based on location.
 Real-Time Enhanced Credentialing Reporting
Real-Time Enhanced Credentialing Reporting
MedTrainer credentialing reports provide the insight and visibility you need to keep processes on track and share data with leadership to make important business decisions. Customize enhanced credentialing reporting with the data and filters you need, then save the reports you use most often and schedule them to email (internally or externally) on a regular basis (daily, weekly, monthly).
Get the big picture of your credentialing process with reports that include all data in MedTrainer Credentialing, including provider demographic information, enrollment and verification data, and more. Some of the most popular uses are:
- Document and license expiration
- Recredentialing timelines
- Enrollment roster set up by payer
- Exclusions status
- Progress on PSV by provider
- Privileges by provider
- Management of multiple locations or specialties
Robust Reporting With MedTrainer
MedTrainer Credentialing Software is built for healthcare organizations who want to manage the credentialing process, but need to get more done in less time.
In addition to credentialing reports, MedTrainer Credentialing Software includes provider profiles, a central location for all credentialing information and documentation. Providers can upload their documents to a secure portal and receive reminders until all required documents are added. Automated license and certification expiration emails are sent to both the provider and credentialer to ensure recredentialing can be completed prior to the deadline.
Have Credentialing Confidence, No Matter What
 Learning
Learning