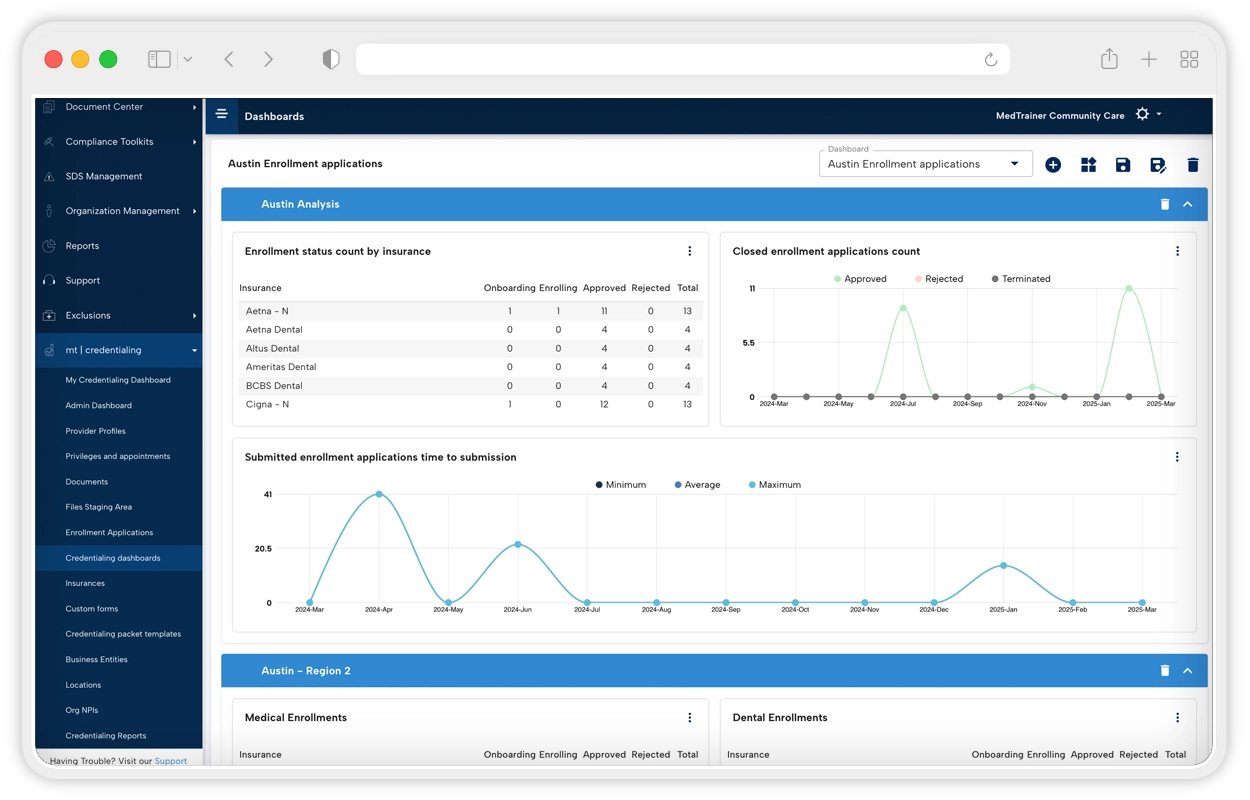
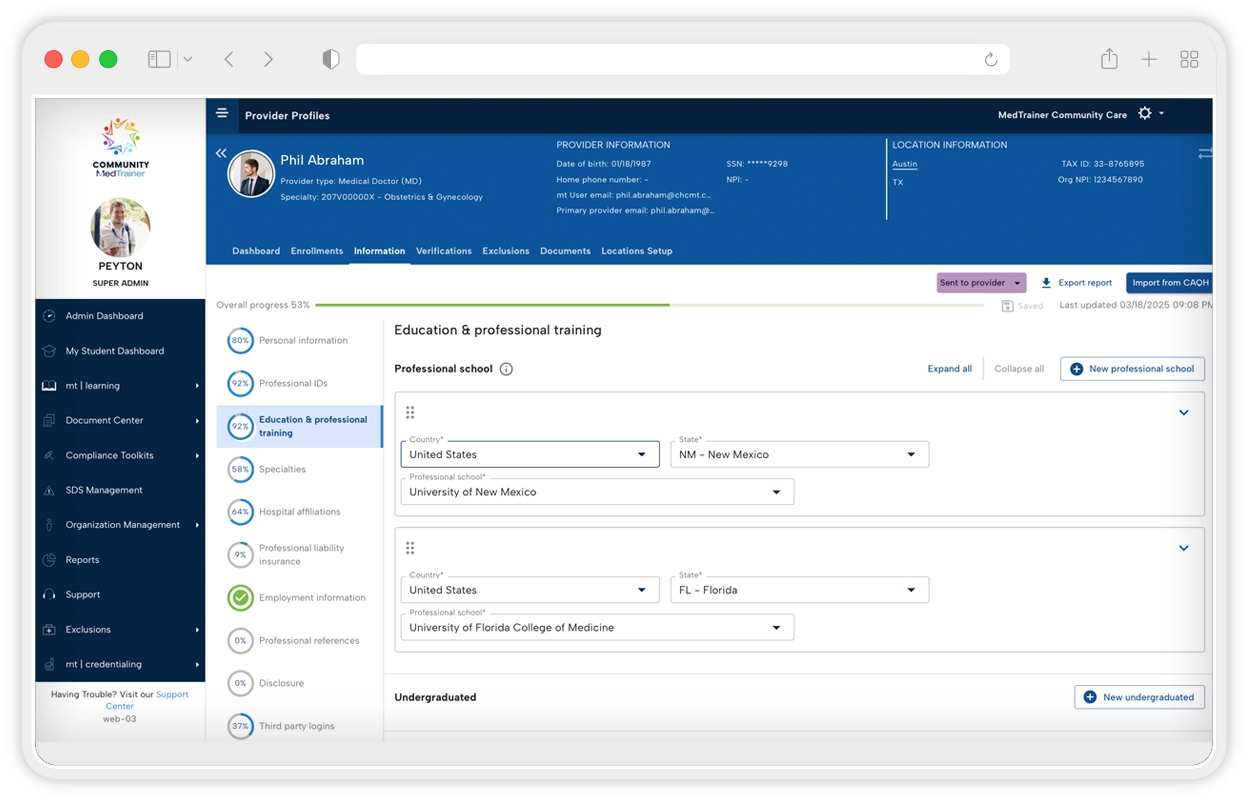
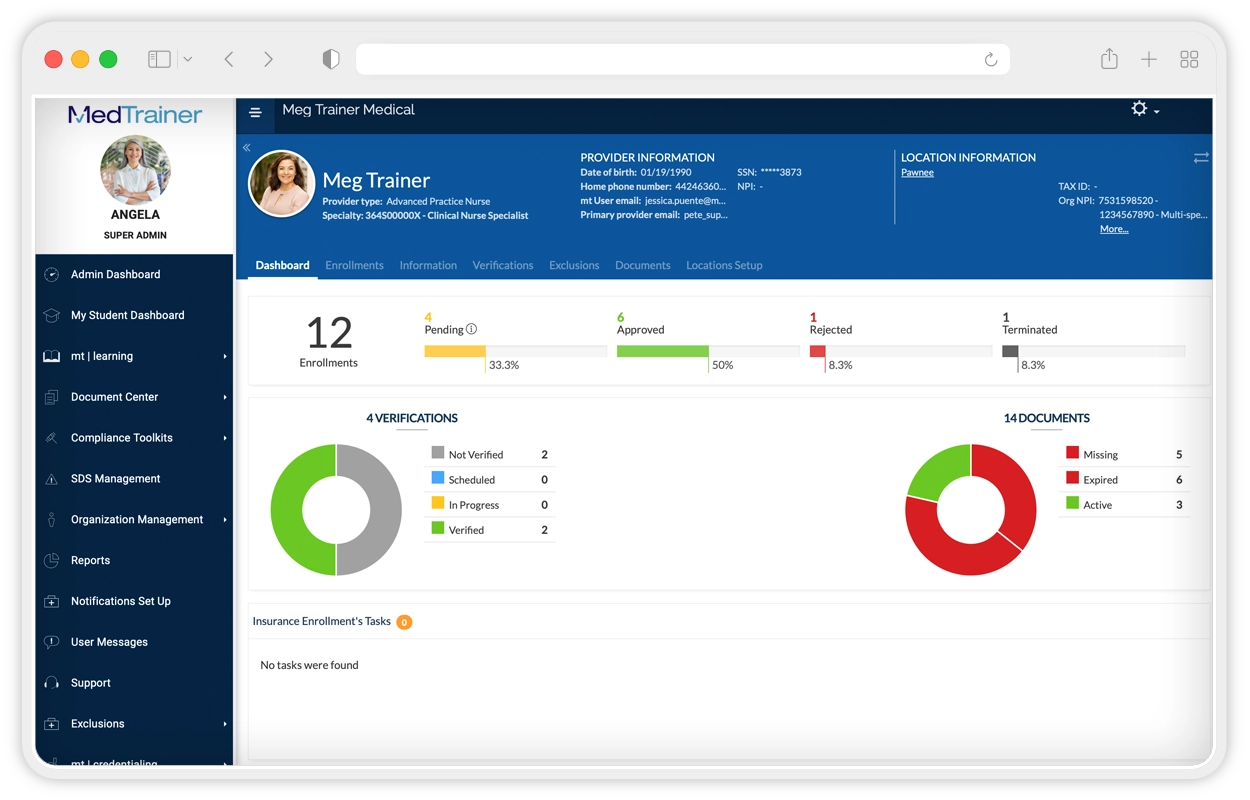
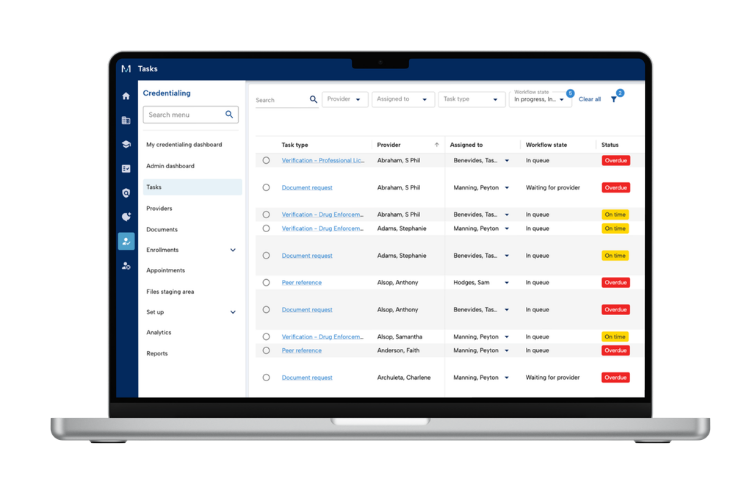
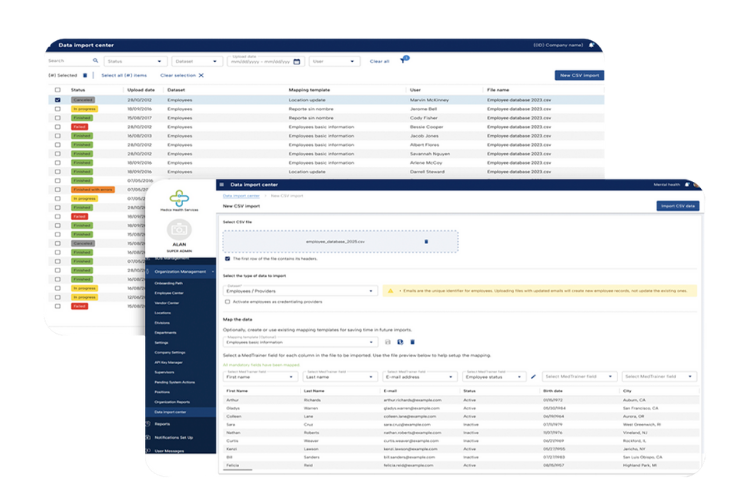
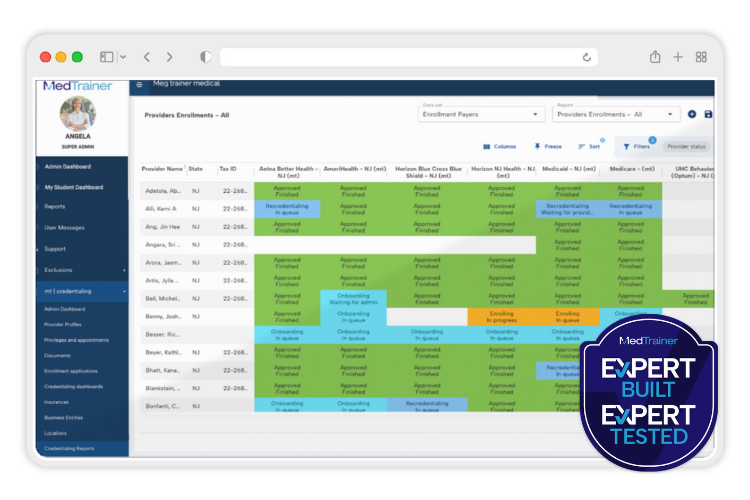
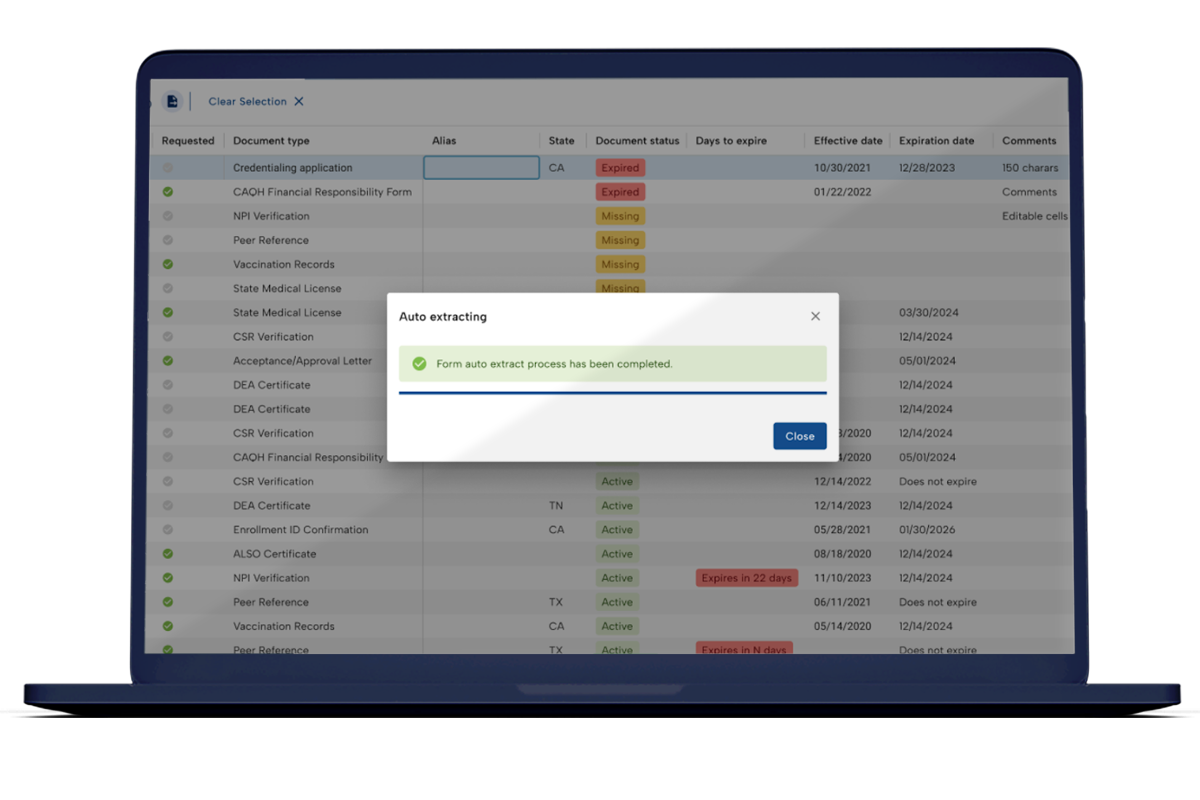
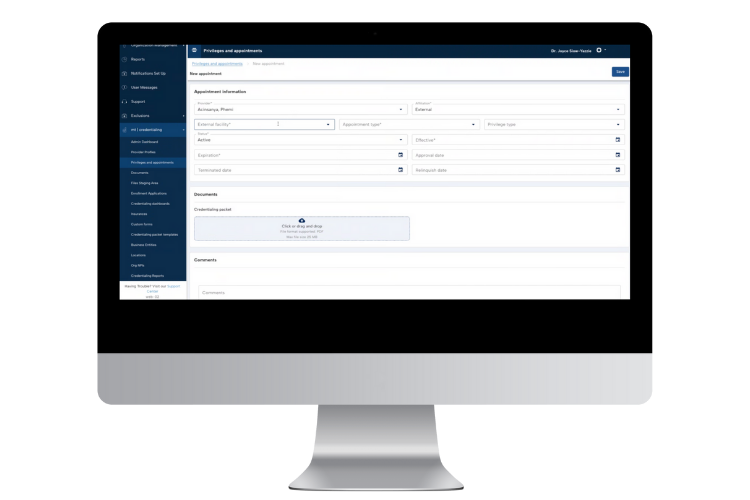
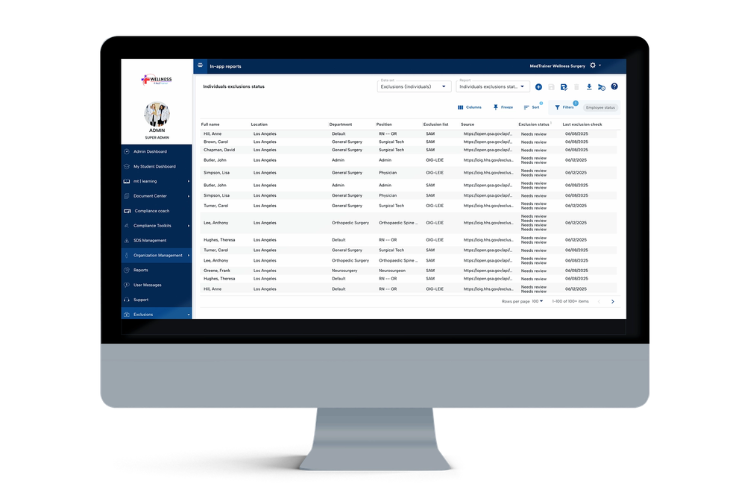
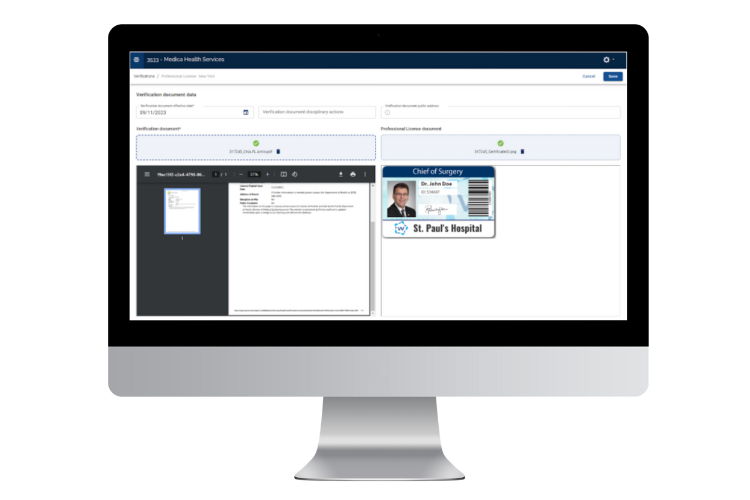
Proven to offer the best tools for streamlining credentialing processes, MedTrainer’s Managed Credentialing Services are ideal for healthcare organizations with 10 or more providers that want to eliminate credentialing backlogs and improve operational efficiency. Medical groups, hospitals, behavioral health networks, dental practices, and multi-location clinics all benefit from our streamlined approach! If your team lacks the capacity or expertise to keep up with payer enrollments, license verifications, and recredentialing cycles, or if delays are stalling your revenue or patient care, healthcare credentialing services can be the game-changer for you.
Our experienced, in-house credentialing team works as an extension of yours, managing every detail while maintaining compliance with NCQA and The Joint Commission standards. If your goal is to speed up provider onboarding, reduce errors, or ensure 100% compliance, MedTrainer’s Managed Credentialing Services provide the scalable, expert-driven support to help you achieve it.
 Learning
Learning