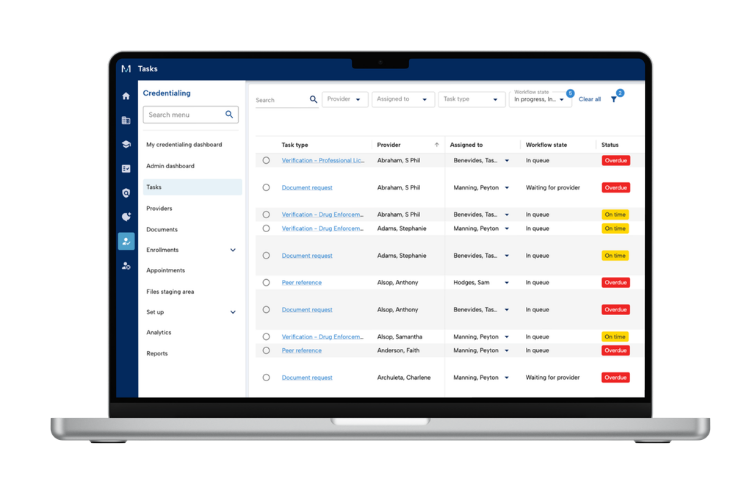
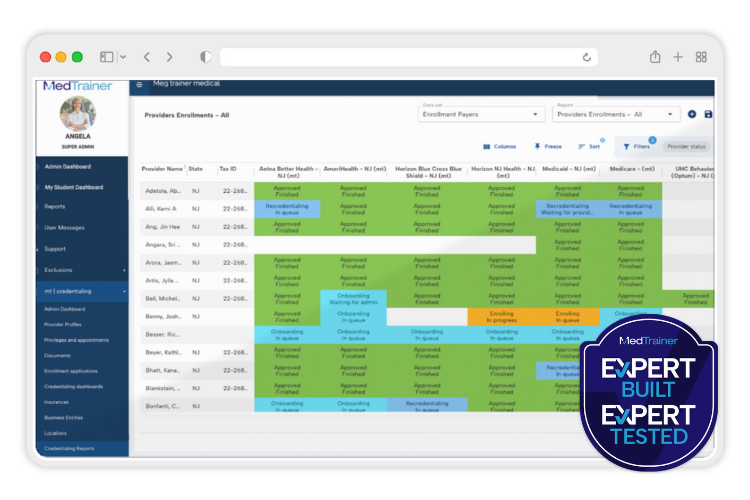
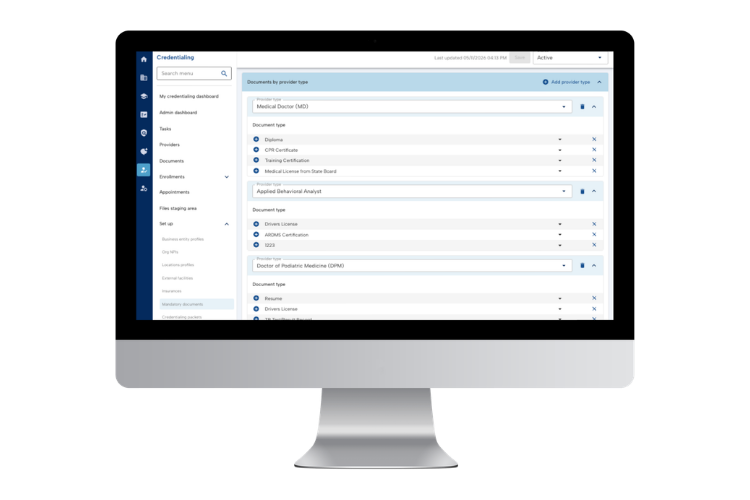
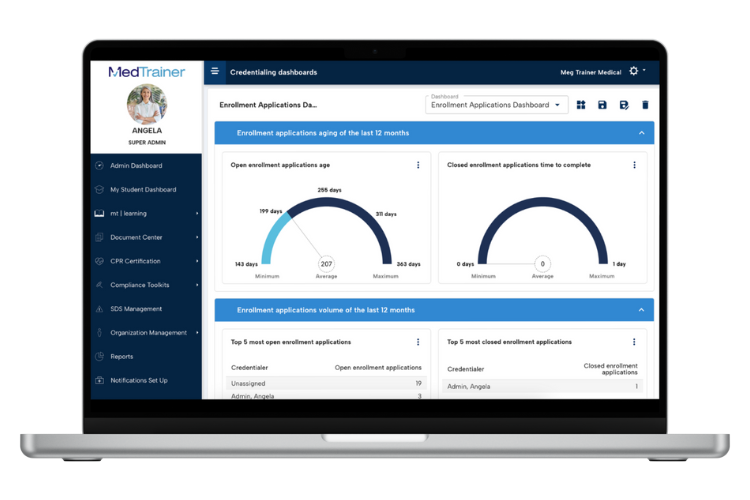
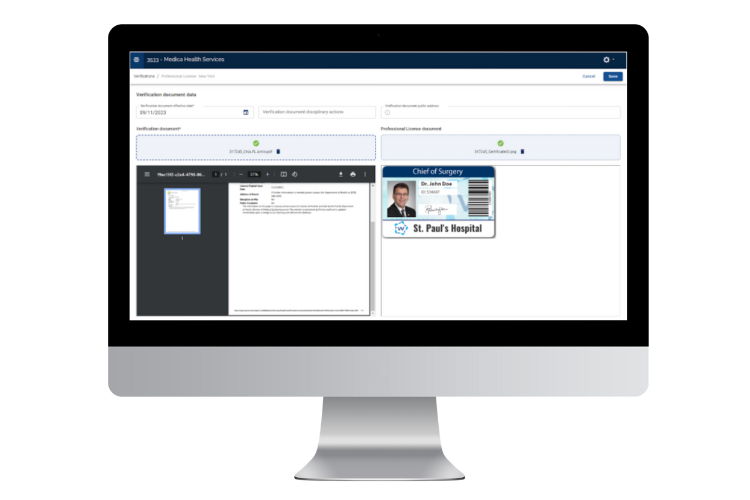
Yes! MedTrainer offers flexible integration options designed to fit a lot of the systems your organization already relies on. Considered among the best names for credentialing software, MedTrainer’s healthcare credentialing management system connects with leading HRIS platforms, including ADP, UKG, Paylocity, Workday, and Dayforce. There are also direct integrations with CAQH, NPDB, OIG, and SAM to eliminate back-and-forth and access the most up-to-date information. You can synchronize provider records, reduce double entry, and ensure accuracy across systems in real time. For many healthcare organizations, these integrations help bridge gaps between credentialing, HR, and operations teams. MedTrainer’s medical credentialing software aligns data across departments, which improves visibility and prevents errors that could lead to delays or compliance headaches. Whether you manage a hospital, dental practice, or multi-site medical group, the healthcare credentialing management software keeps everyone working from the same reliable provider data. It’s a simpler, cleaner way to connect systems. And it saves hours of administrative work!
 Learning
Learning