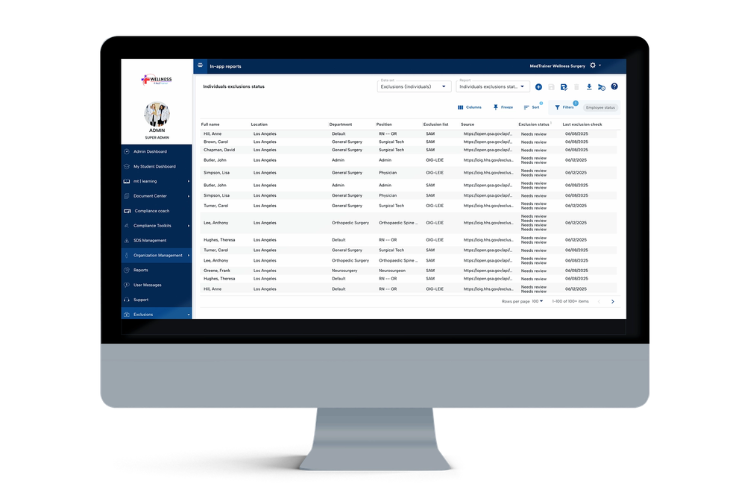
It’s overwhelming to check multiple exclusion databases for every provider every month. But, conducting continuous DMF, OIG, SAM, and state exclusions checks is one of the most important precautions a healthcare organization can take to protect its reputation and revenue. So how do you balance the need for exclusion checks with the time required?
Using automated exclusion list software.

Beyond the Primary Source Integrating Continuous Monitoring Into Your Credentialing DNA
Automating this process can significantly reduce the risk of compliance violations and improve operational efficiency. In this post, I will explore the importance of exclusion checks, the challenges of doing them manually, and how automation can simplify the entire credentialing workflow.
An exclusion list (the primary exclusion list for healthcare industries) contains individuals or entities that are excluded from practicing healthcare and receiving federal healthcare payments due to criminal behavior or misconduct
Why Healthcare Organizations Must Check Multiple Exclusion Lists
Compliance teams must regularly check multiple exclusion lists to avoid employing individuals or entities barred from federal or state healthcare programs. Missing even one exclusion source can lead to financial penalties, repayment obligations, and reputational damage.
Healthcare organizations typically need to check several exclusion sources, including:
-
OIG (Office of Inspector General) – LEIE
The OIG List of Excluded Individuals and Entities (LEIE) identifies providers and organizations excluded from participating in federal healthcare programs due to fraud, abuse, or other misconduct. -
SAM (System for Award Management)
SAM tracks individuals and organizations suspended or debarred from federal contracting and federal funding programs. -
DMF (CMS Preclusion / Death Master / other DMF databases depending on context)
DNF databases flag individuals who are deceased or otherwise prohibited from participation in healthcare programs. -
State Medicaid Exclusion Lists
Many states maintain their own exclusion lists for providers barred from participating in state Medicaid programs.
Together, these checks help organizations ensure they are not employing individuals who are prohibited from providing services or receiving reimbursement through federal or state healthcare programs.
Challenges of Manual Exclusions Monitoring
Clearly conducting DMF, SAM, and OIG exclusion checks is critical, but when you’re doing it manually, it’s error-prone and tedious.
Healthcare organizations typically need to check multiple exclusion lists such as OIG, SAM, DMF, and state Medicaid exclusions for every person on staff, every month (according to NCQA guidelines). Each list requires separate searches and verification, as well as documentation of results for audit purposes.
Since you likely face interruptions, it can take a full day to find, verify, and track 20 employees. If you have 100 employees, that’s suddenly an entire week of work! These interruptions also make mistakes more likely. It’s easy to skip someone or enter the wrong information into your spreadsheet.
If you hire an excluded provider, you’ll be punished even if you are unaware of the exclusion.
Missed or incorrect exclusion checks can also result in compliance breaches, potential audits, and the financial and reputational damage that comes with these violations. As the healthcare industry becomes more complex, manual exclusion checks become outdated, and the risk of non-compliance increases.
How Automation Transforms Exclusion Checks
Automation is a major advancement when it comes to exclusion checks. Automated systems streamline the entire process, eliminating manual searches, data entry, and tedious tracking. Selected databases are automatically checked on an NCQA-approved schedule with the results logged and notifications when an employee’s status changes.
When exclusion checks are part of healthcare credentialing software, they’re integrated directly into the workflow, ensuring a faster, more accurate process.
Automated exclusions monitoring offers several benefits over manual checks:
Real-Time Updates
Get notifications when an employee’s exclusion status changes so you can immediately investigate.
Bulk Processing
Instead of completing exclusions screening one by one, automation processes all individuals and entities at once, saving valuable time and resources.
Tracking and Reporting
Automated systems track every exclusion check for every individual and entity, so you can easily demonstrate compliance. Easily customize and save a report that shows all the information an auditor will need.
Even if part of the process is automated, organizations still face inefficiencies if their tools only check one or two databases. True automation requires software that monitors all required exclusion sources in one place, otherwise teams still spend hours navigating multiple websites and manually tracking results.
Benefits of Automated Exclusion Checks
Implementing automated DMF, OIG, SAM, and state exclusions exclusion checks offers a host of benefits that can improve both healthcare compliance and operational efficiency. Here are some of the key advantages:
Time and Resource Savings
Automated exclusion checks dramatically cut down on the staff time needed for this manual task. It allows employees to focus on higher priorities that drive revenue, such as preparing credentialing packets and enrolling providers.
Always Compliant
Automated systems continuously monitor exclusion lists so organizations have the most up-to-date information. This helps avoid costly healthcare compliance violations and the risks associated with hiring excluded professionals.
Increased Efficiency
Automation speeds up the healthcare credentialing process, leading to faster new hire onboarding and fewer delays. With bulk processing and real-time updates, organizations can manage exclusions efficiently, ensuring that they maintain compliance without sacrificing productivity.
Simple Reporting
Automated systems typically include robust reporting features that track exclusion status changes, generate audit-ready reports, and flag potential issues. Easily sort and filter reports by individual, location, last exclusion check date, and more.
Implementing Automation for Multiple Exclusion Lists in Your Organization
Once you consider your current processes and find the right solution, adopting automation for DMF, OIG, SAM, and state exclusions exclusion checks should be seamless and will allow your organization to jump right in and learn quickly. Here are some steps to implement automation in your organization:
Evaluate Your Current Processes
Assess your existing exclusions monitoring workflow to determine how long it takes each month. Equate that time to dollars — how much does your current process cost in staff time? Then compare it with the cost of software.
Be sure to take into account errors or mistakes in your current process that have been costly for the organization.
Choose the Right Software
Look for solutions that work well with your healthcare credentialing software and process. Many organizations opt for a comprehensive credentialing solution that includes automated exclusion checks, credentialing workflows, automated license verification, enrollment tracking, customizable reporting, and more.
At a minimum ensure your chosen solution tracks every OIG exclusion list check, with real-time reporting for audit purposes.
Train Your Staff
Once you’ve chosen the right solution, train your team on how to use it effectively. Establishing clear protocols for using the software and monitoring for updates is essential to ensure smooth implementation.
Monitor and Optimize
After automation is in place, continuously monitor the process and make adjustments as needed. This includes reviewing reports, tracking compliance, and ensuring that OIG exclusion checks are up-to-date.
Simplify Exclusions Monitoring With MedTrainer
Automating DMF, OIG, SAM, and state exclusions exclusion checks is a powerful way to streamline credentialing processes, improve compliance, and protect your organization from potential legal and financial risks. MedTrainer tracks all of these sources automatically on a recurring schedule, making sure your organization always has the most current exclusion data without the manual work.
If you’re looking to ditch the old-school workflows and stay ahead of compliance challenges, you need MedTrainer’s automated exclusion monitoring.
Automation protects your organization and enhances operational efficiency, helping you focus on what truly matters — providing safe, high-quality care to your patients.
Ready to streamline your credentialing process with automated DMF, OIG, SAM, and state exclusions exclusion checks? Learn more today!
 Learning
Learning