Compliance is critical in the medical field, especially during times of high healthcare staff turnover. Even as people and roles change, compliance guidelines stay the same, and serve to help healthcare organizations adhere to legal, ethical, and regulatory standards.
Yet, where there’s a high staff turnover rate, there’s also an increased risk of errors and deviations from established protocols. Almost always, it results in negative consequences for patients and the organization alike. By prioritizing steadfast compliance, healthcare organizations can minimize the risk of these incidents, to protect patients and their reputation in times of change.
Here’s how to make sure compliance isn’t just a box you’re checking, but a core value that’s top-of-mind at all times — especially during times of turnover.

WEBINAR: Adapting To Overcome Healthcare Staff Turnover
The Costs of High Healthcare Turnover
It’s well-known that healthcare staff turnover is costly, but it’s difficult to imagine how far the rippling effects truly travel. Lost productivity, financial strain, increase in incidents or errors, and a worse patient experience are all outcomes that result from high turnover rates — each with its own cost factor.
There are also costs that accompany time-to-fill and time-to-productivity, two critical human resources metrics. It takes up to two years for an employee to become fully productive, and replacing a staff member can cost up to 33% of the position’s annual salary. As new staff learns processes, policies, and equipment, errors can and will occur.
These (and countless peripheral) costs emphasize the need for healthcare organizations to prioritize the employee experience to ensure the industry’s long-term health. And, in retaining quality candidates, make sure they’re trained against best practices that equate to high standards of quality.
Why Medical Professionals Are Leaving in Droves
Healthcare staff turnover is a very real issue causing significant challenges in not only staffing at capacity, but finding and retaining qualified and experienced caregivers. Here are the primary reasons why:
- Aging Nursing Population. Long-tenured nurses are choosing to retire as the stress of healthcare delivery rises post-pandemic. They’re leaving a shortage of experienced professionals in their wake.
- Low Pay. Despite the critical importance of their roles, nursing salaries are still stagnant or below average in many states. Moreover, high-paying travel nursing and locum tenens positions are drawing nurses in droves.
- Lack of Advancement Opportunities. A recent Pew Research Center survey found that a lack of opportunities for advancement is a top concern among professionals who choose to leave their field.
What can we do to address this trend? It’s a question many healthcare compliance leaders ask themselves as they strategize methods to keep turnover from affecting patient care. It’s a complex problem that has a multifaceted answer larger than any single facility can solve. That said, compliance managers have more power than they think to affect positive results among their own staff.
4 Compliance-Related Adjustments to Help Manage Healthcare Staff Turnover
Leadership is the (hopefully) constant variable amidst change, and it falls to management to ensure compliance standards are at the core of training and practice.
You already know that compliance is critical for maintaining high standards of patient care and protecting the reputation of the organization. But how can you build a culture of safety into the core of everyday operations?
Here are four adjustments you can make, starting with your newest hires:
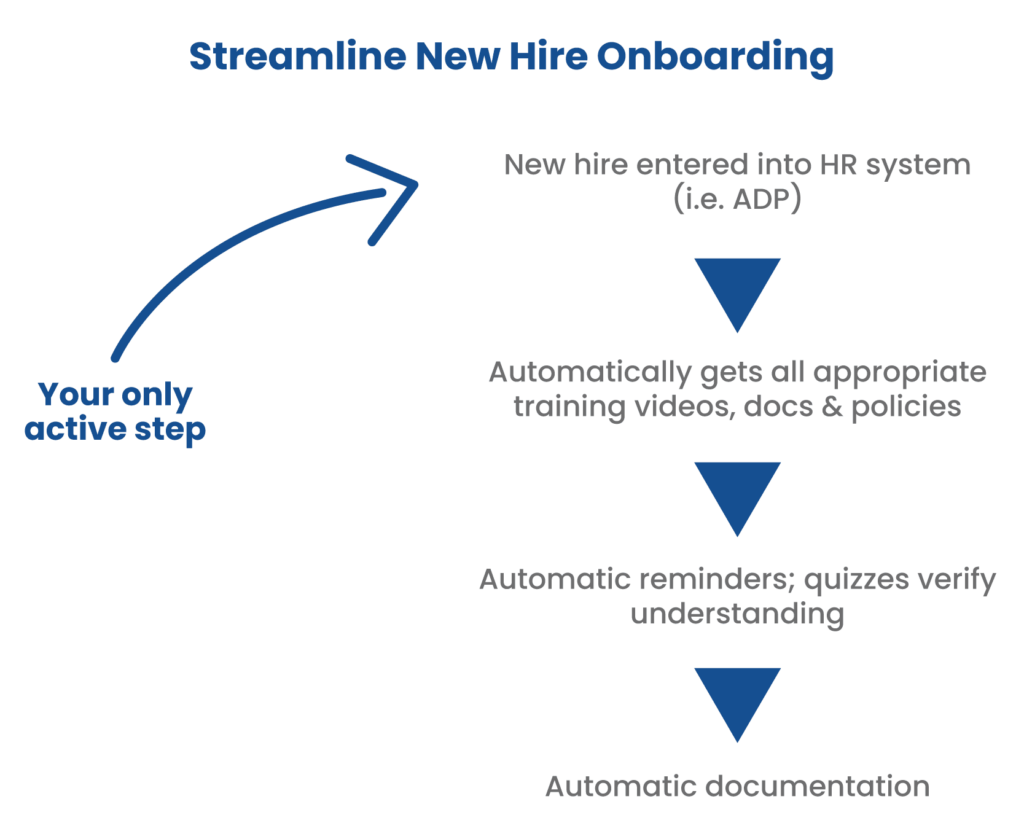
1. Nail the Onboarding Process
A 2022 survey by MedTrainer found that small to medium-sized healthcare organizations onboard an average of 28 new staff members annually, with the smallest businesses onboarding over 25% of their total staff each year.
Proper and timely onboarding can improve staff productivity by over 70% and employee retention by 82%! A well-planned onboarding program that provides support over the first 6 to 12 months can help new hires ramp up their performance faster and contribute more to the organization.
As a compliance officer, you have to ensure these new employees are fully compliant, which involves mandatory training, policy acknowledgments, and credentialing. An all-in-one compliance platform simplifies the process by grouping policies and training for electronic acknowledgment and automatic reminders.
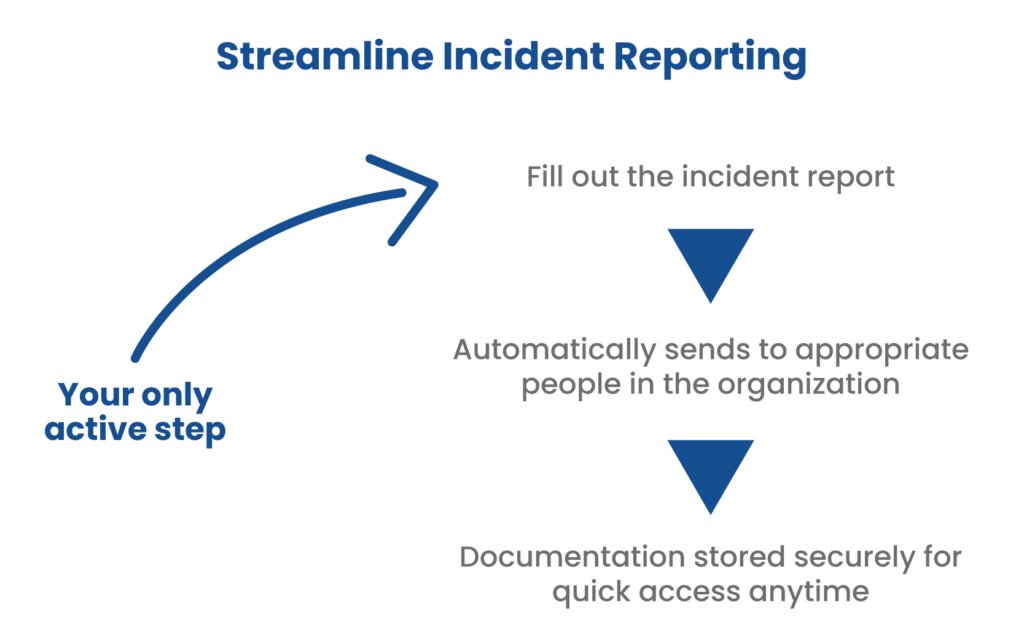
2. Emphasize Incident Reporting
As turnover increases, incident rates tend to rise. This is largely due to new employees not being familiar with their work environment or policies. To improve safety, it’s important to consistently report incidents and use the information to improve new hire training.
Using a non-confrontational approach for incident reporting can lead to productive dialog and process improvement, and it’s helpful to streamline and document the process to track progress.
Here again, hospital leadership can use an all-in-one compliance platform to customize incident report templates, automate escalation, and analyze trends for greater infection prevention. Including incident reporting guidance in your infection control plan is a key measure for prevention.
3. Streamline Credentialing
An already lengthy and expensive process, credentialing can cause significant time and financial losses for healthcare organizations. Don’t give new caregivers a reason to leave before they even see a patient! Credentialing providers more quickly is a win for the provider and organization by maintaining a smooth revenue flow and reducing the risk of lapses that lead to billing problems.
Accelerating the enrollment process by organizing tasks and workflows, automating application completion and notifications, and providing drillable reporting can also improve progress tracking. Automating the whole process can save time and improve efficiency, including data import, exclusion list monitoring, and verifications for professional licenses and certifications.
4. Make Workplace Safety a Priority
Alleviate the strain of healthcare staffing shortages and reduce return visits and care protocols by making workplace safety a priority. Creating a healthy hospital culture and emphasizing safety creates a welcoming environment that makes healthcare personnel more comfortable coming to work each day.
All employees need access to essential documents, policies, and safety data sheets for reference at any time, including during inspections. As the number of new employees increases, safety data sheet management becomes more important and needs to be accessible — rather than stored on paper in a filing cabinet. Learn more about document policy and compliance.
The Time for Improvement is Now
Compliance can be a tool to improve healthcare staff turnover and combat the industry’s staffing shortages. The temptation to let things slide in the face of staffing challenges may be strong, but doing so can result in decreased safety, leading to violations and potential penalties.
Compliance teams can’t do it on their own. A high turnover rate increases the likelihood of incidents and exponentially increases the training “check boxes.” A robust compliance program helps to streamline tasks by keeping important documents accessible and fostering a culture of safety.
In short, a commitment to compliance is a commitment to safety and quality care, and it’s a priority that can’t be ignored.
 Learning
Learning