Credentialing is the backbone of provider onboarding. But it can also be one of the biggest sources of organizational slowdowns. At MedTrainer, we know this because we live it too. Our credentialing services team manages more than 10,000 providers across the country, giving us a front-row seat to the same challenges healthcare organizations face every day.
To better understand these challenges, we surveyed our credentialing team leaders, asking them what typically halts and helps the process. Their feedback confirmed what many in the industry already know: the biggest slowdowns often come from limited visibility and cumbersome provider documentation.

Credentialing Visibility To Improve Your Bottom Line
The findings below illustrate how visibility gaps and documentation hurdles create slowdowns, what healthcare organizations often prioritize most, and how MedTrainer helps teams turn those challenges into opportunities for speed and accuracy.
Why Enrollment Visibility Tops the Credentialing Wish List
In our survey, 92% of MedTrainer credentialing teams said the number one client request is payer enrollment status by provider and location. It makes sense! Leaders want visibility into enrollment status by provider and location, because those data points tie directly to staffing decisions – like which providers can see which patients – revenue forecasts, and more.
Organizations are left guessing when they don’t have transparency, And we all know that when revenue is on the line, guesswork won’t cut it. Knowing exactly where providers stand is critical to both revenue and operations.
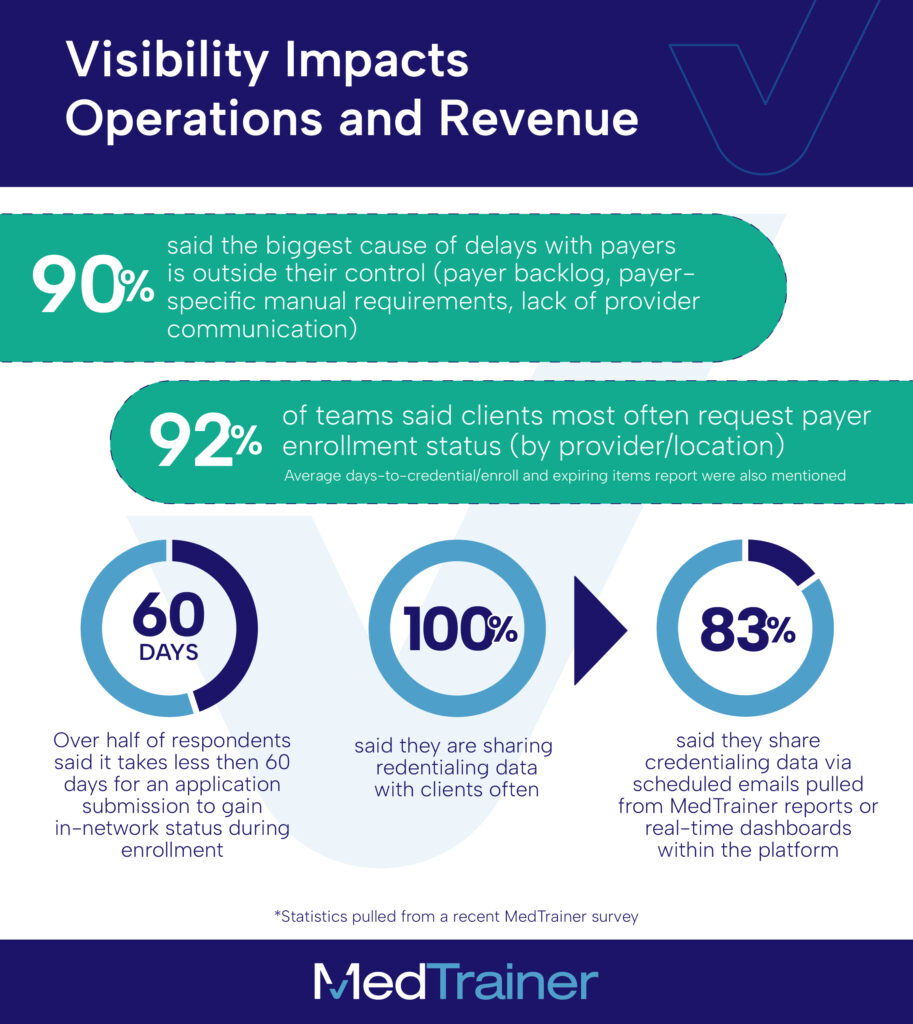
At the same time, the majority of MedTrainer specialists told us that payer delays outside their direct control are the biggest problem. Backlogs and payer-specific requirements may be unavoidable, but what teams can control is how they react. That’s where visibility into the credentialing process changes the game.
MedTrainer transforms uncertainty into clarity by giving healthcare organizations and their leaders visibility into the data that matters most. Dashboards not only track enrollment status by provider and payer, but also surface benchmarks like average time to decision per payer. That means leaders can spot when one payer is lagging behind or when denials spike.
Even when payers or other external players slow things down, healthcare organizations don’t lose momentum. MedTrainer includes automated reminders to follow up with payers, because as we all know, it’s the squeaky wheel that gets the grease. Pre-set credentialing packet templates specific to each provider also help guarantee the right documentation is there the first time.
These tools keep credentialing cycles on track, reduce preventable slowdowns, and give organizations confidence that providers will be ready for patients as planned.
Credentialing Moves at the Speed of Documents
Credentialing can only move as fast as the flow of provider documentation. And our internal survey confirmed what credentialing specialists live every day: collecting provider documents is often the single most time-consuming stage of the process. Missing or outdated files often stall onboarding before it even begins.
The survey also showed that work histories and CVs are consistently the hardest items to obtain, followed closely by malpractice insurance and education certificates. These bottlenecks can stall payer applications, push back start dates, and slow down revenue.
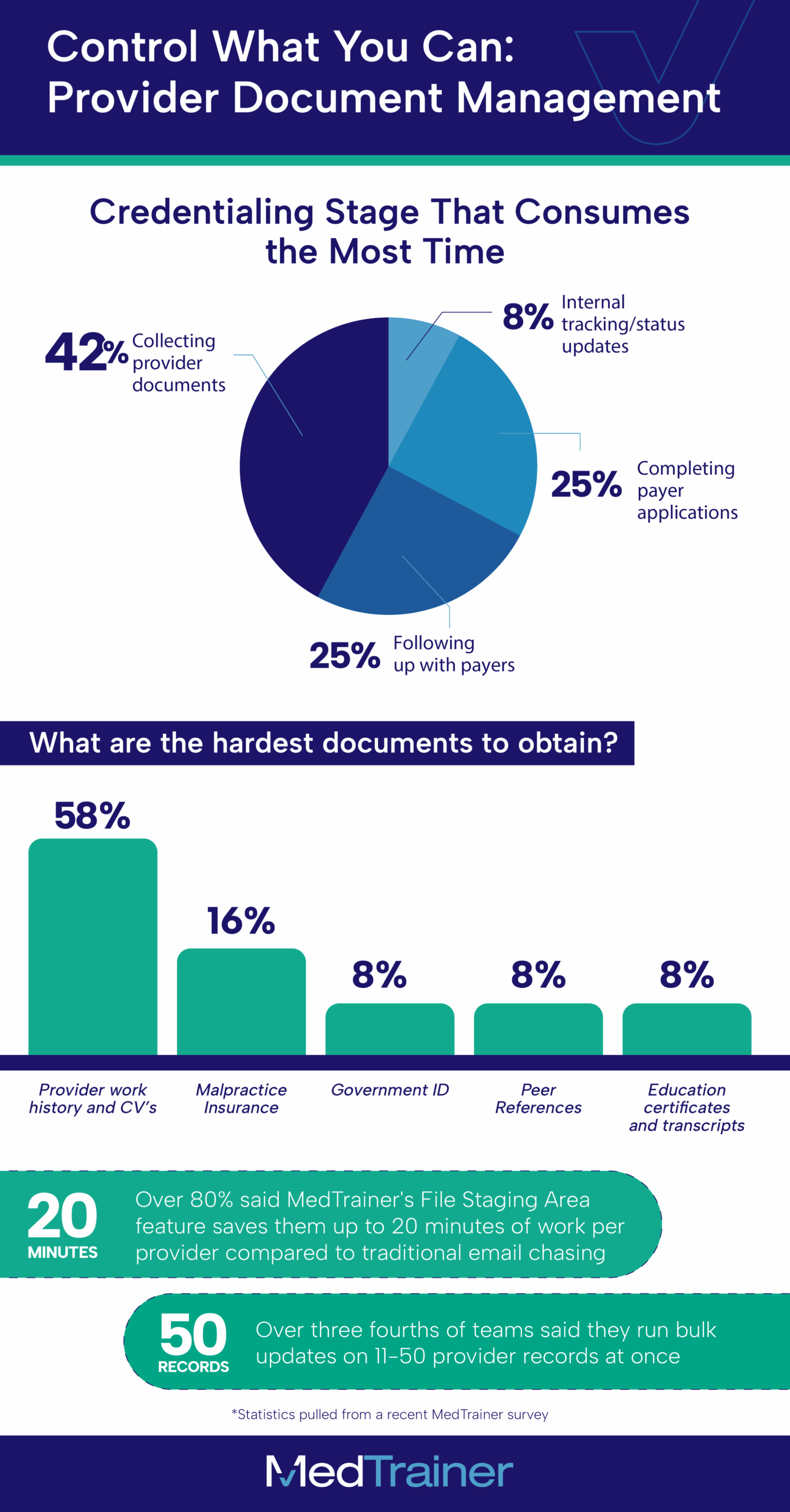
With MedTrainer, these bottlenecks become manageable. See how our team uses the platform, including these MedTrainer tools that make a measurable difference for our credentialing specialists:
File Staging Area: This AI-powered intake system sorts incoming documents automatically. Instead of credentialers spending 20 minutes per provider manually opening files, renaming them, and dropping them into the right folder, the system classifies, extracts key data, and places each file directly into the provider’s profile.
Bulk Updates: Credentialers often need to update dozens of provider records at once. The bulk update functionality allows them to process 30, 40, even 50 records in a single swoop, rather than repeating the same manual steps provider by provider. Those minutes translate into hours of regained productivity. Add in bulk updates across multiple records, and the slowest part of credentialing suddenly moves at speed.
Credentialing With Confidence
Innovation at MedTrainer goes far beyond rolling out the latest feature. It’s about listening to healthcare organizations like yours, learning from the credentialing challenges our own team encounters every day, and improving continuously to meet evolving needs.
Because our specialists manage credentialing for thousands of providers, the same obstacles you face are the ones we see and solve firsthand. That’s why you can be confident MedTrainer isn’t just another platform. It’s a solution built and enhanced by experts who live credentialing right alongside you.
 Learning
Learning